Everything to Know about Psoriasis
Everything to Know about Psoriasis
Psoriasis is a chronic skin condition resulting from an overactive immune system that causes overly rapid skin cell turnover. This often leads to patches of thick, scaly skin on various parts of the body. Psoriasis has no cure, but managing your condition begins with understanding more about it.
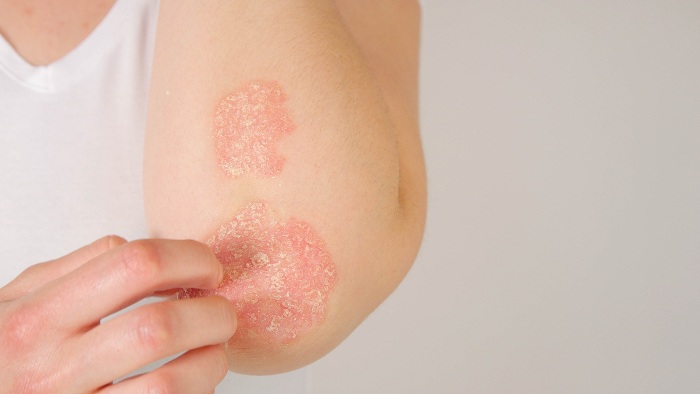
Symptoms of Psoriasis
This skin condition manifests in many ways. Symptoms become most severe during a flare-up, the severity of which varies widely from person to person. The most common symptoms include:
- Red patches of skin covered with thick, silvery scales
- Dry, cracked skin that may bleed
- Itching, burning, or soreness in the affected areas
- Thickened, pitted, or ridged nails
- Swollen and stiff joints, especially in the morning or after periods of inactivity
Types of Psoriasis
Psoriasis comes in many forms, each having distinct characteristics:
- Plaque psoriasis is the most common, characterized by raised, inflamed, red skin covered with silvery-white scales. It is often found on the elbows, knees, and scalp.
- Inverse psoriasis causes smooth, red patches in the folds of the skin and is worsened by friction and sweating.
- Erythrodermic psoriasis is a rare and severe type covering the entire body with a red, peeling rash that can itch or burn intensely.
- Guttate psoriasis often starts in childhood or young adulthood, appearing as small, water-drop-shaped sores on the trunk, arms, and legs.
- Pustular psoriasis is a rare type that appears as white blisters of non-infectious pus surrounded by red skin.
- Scalp psoriasis appears on the top of the head, often extending beyond the hairline. Symptoms range from minor scaling to thick, crusted plaques.
- Nail psoriasis affects the fingernails and toenails, causing discoloration, pitting, and abnormal nail growth, which can become painful.
Diagnosing Psoriasis
Several steps are involved to diagnose psoriasis correctly:
- Physical examination: A dermatologist examines the affected skin, scalp, or nails.
- Skin biopsy: A small skin sample may be sent for examination under a microscope to confirm the diagnosis and rule out other skin disorders.
- Joint examination: If joint pain is a symptom, a rheumatologist may assess the joints to determine whether the condition is developing into psoriatic arthritis.
Causes and Triggers of Psoriasis
Psoriasis is primarily an autoimmune condition. Certain factors can trigger its onset or exacerbate existing conditions:
- Immune system: Overactive T cells attack healthy skin cells, mistaking them for pathogens. This leads to excessive skin cell growth, which builds and forms the plaques associated with psoriasis.
- Injuries: Cuts, burns, and insect bites irritate psoriasis.
- Stress: High stress levels and anxiety attacks can trigger a flare-up.
- Weather: A cold, dry environment can worsen symptoms.
- Medications: Certain medications, like lithium, beta-blockers, and antimalarials, can trigger a psoriasis flare-up.
Risk Factors for Psoriasis
Various factors can increase the risk of developing psoriasis or exacerbate existing conditions:
- Inflammatory bowel disease (IBD): Conditions like Crohn’s disease and ulcerative colitis increase the risk of developing psoriasis.
- Genetic factors: Individuals with a family history of psoriasis are more likely to develop this skin condition.
- Infections: Strep throat, HIV, and other infections may trigger the onset of psoriasis.
- Obesity: Excess weight increases the risk and may also make symptoms more severe.
- Smoking: Heavy smokers have a higher risk.
Complications of Psoriasis
Untreated psoriasis can lead to other health issues affecting the bones, muscles, and metabolic system. Most notably, about one in three people with psoriasis develop psoriatic arthritis within five to 10 years of their diagnosis. This lifelong autoimmune disorder is characterized by joint pain, stiffness, and swelling.
People with psoriasis are also more likely to develop:
- Depression and anxiety
- Cardiovascular disease
- Metabolic syndrome
- Inflammatory bowel disease
- Obesity
- Dyslipidemia
- Diabetes
- Some types of cancer
Treatments for Psoriasis
Managing psoriasis often requires a multifaceted approach, including:
- Medications: Methotrexate and cyclosporine are often prescribed to treat psoriasis. Biologic drugs that alter the immune system may also be effective.
- Topical therapies: Corticosteroids reduce inflammation and itching, while Vitamin D analogs slow skin cell growth.
- Systemic therapies: These oral or injected medications work throughout the body to suppress the immune system and slow skin cell turnover.
- Phototherapy: UVB light treats psoriasis lesions, slowing the growth of affected skin cells.
Preventing Psoriasis
Preventing flare-ups and managing symptoms requires the following:
- Daily bathing with mild soap
- Regular moisturizing
- Meditation, yoga, or deep breathing exercises to manage stress
- Balanced diet and regular exercise
- Limiting your alcohol consumption and quitting smoking
- Identifying and avoiding personal triggers
Frequently Asked Questions about Psoriasis
What are three symptoms of psoriasis?
- Red patches of skin covered with silvery scales
- Dry, cracked skin that may bleed
- Itching or soreness around the affected areas
Is psoriasis contagious?
No. Psoriasis is an autoimmune disorder primarily caused by genetics and other triggering factors.
What causes psoriasis to flare up?
Stress, certain medications, infections, injuries to the skin, and cold weather can trigger flare-ups.
Contact Divine Dermatology for Psoriasis Care
Divine Dermatology in Fort Collins, Loveland, and Longmont, CO, integrates state-of-the-art dermatology with other medical disciplines to manage psoriasis effectively. Our commitment to long-term skincare health ensures that each patient receives a well-thought-out treatment plan. Contact us at 970-286-2668 to receive a diagnosis and begin caring for your skin condition.


